Back pain that persists for weeks or worsens with movement may sometimes indicate a structural injury within the spine. One condition that requires prompt evaluation is a Lumbar Pars Fracture, San Antonio, TX, a stress fracture affecting a specific part of the lower spine. Patients experiencing persistent lower back pain—especially athletes, adolescents, or individuals involved in repetitive physical activity—may be dealing with this condition without realizing it.
At the Brain and Spine Institute, San Antonio, Texas, advanced diagnostic tools and personalized treatment plans are used to help patients recover from spinal injuries. Under the care of Dr. Osama Ahmed, patients receive expert evaluation and comprehensive treatment options for lumbar spine injuries in San Antonio.
This guide explains the causes, symptoms, diagnosis, and available treatment approaches for lumbar pars fractures, so patients can better understand their condition and treatment options.
Understanding Lumbar Pars Fractures
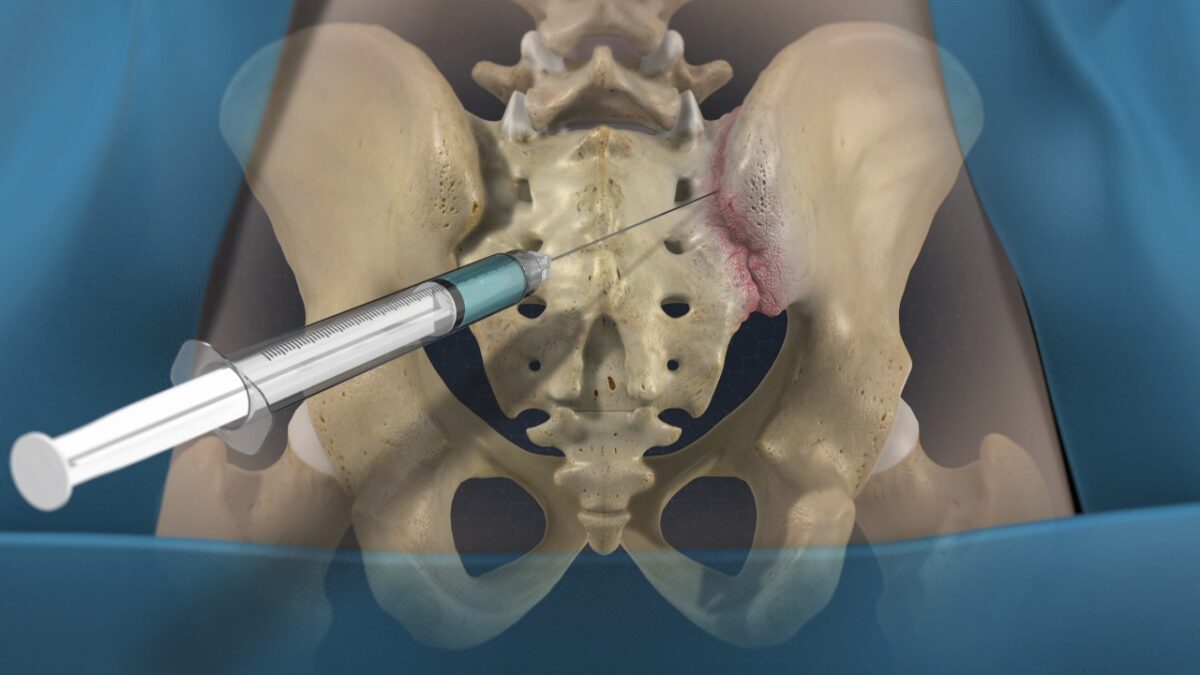
A lumbar pars fracture refers to a break or stress fracture in the pars interarticularis, a small section of bone that connects the upper and lower joints of a vertebra. This region is located in the lower spine (lumbar spine) and plays an important role in stabilizing spinal movement.
When the pars interarticularis becomes weakened due to repetitive stress, trauma, or overuse, a fracture can occur. In some cases, this injury can lead to a condition known as spondylolysis, and, if severe, it may progress to spondylolisthesis, in which one vertebra slips forward over another.
Seeking early professional treatment for a lumbar spine fracture in San Antonio can prevent complications and help restore normal spinal function.
Common Causes of Lumbar Pars Fractures
Several factors contribute to the development of lumbar pars fractures. Understanding these causes can help patients identify risk factors and seek early care.
Repetitive Spinal Stress
Activities involving frequent bending, twisting, or extension of the lower back can place repeated stress on the pars interarticularis. Over time, this stress may cause small cracks that eventually lead to a fracture.
Athletes in sports such as:
- Gymnastics
- Football
- Weightlifting
- Cricket
- Tennis
Sports Injuries
High-impact sports and sudden spinal movements may directly injure the lumbar spine. Young athletes often experience stress fractures because their bones are still developing.
Degenerative Changes
Age-related degeneration in the spine can weaken vertebral structures. Although pars fractures are more common in younger individuals, adults with degenerative spinal conditions may also develop them.
Trauma or Accidents
Falls, car accidents, or direct trauma to the lower back can sometimes cause fractures in the vertebrae, including the pars interarticularis.
Consulting a Spine fracture specialist in San Antonio, TX ensures accurate diagnosis and effective management.
Symptoms of a Lumbar Pars Fracture
Symptoms vary depending on the severity of the fracture and whether surrounding structures are affected. Some patients may initially ignore symptoms, thinking they are experiencing simple muscle strain.
Common symptoms include:
Persistent Lower Back Pain
Pain in the lower back is the most common symptom. It often worsens during physical activity and improves with rest.
Pain During Movement
Activities such as bending backward, twisting, or lifting heavy objects may intensify discomfort.
Muscle Tightness
Tight hamstrings and stiffness in the lower back frequently accompany lumbar pars fractures.
Limited Mobility
Some patients experience difficulty standing upright or performing everyday movements.
Radiating Pain
In more advanced cases, pain may radiate to the buttocks or legs if nerve irritation occurs.
If these symptoms persist for several weeks, it is important to consult a Lumbar spine specialist in San Antonio, TX, for further evaluation.
How Lumbar Pars Fractures Are Diagnosed
Accurate diagnosis is essential for determining the most appropriate treatment plan.
At specialized spine centres, physicians typically perform several diagnostic steps.
Physical Examination
A detailed physical exam helps assess spinal mobility, pain points, posture, and neurological function.
Imaging Tests
Advanced imaging helps confirm the presence of a fracture and determine its severity.
Common diagnostic tools include:
X-rays – Often the first imaging test used to detect fractures.
CT scans – Provide detailed images of bone structures to identify stress fractures.
MRI scans – Help evaluate soft tissue damage, nerve involvement, and inflammation.
These diagnostic tools allow a Spine fracture specialist in San Antonio, TX, to determine the best course of treatment.
Non-Surgical Treatment Options
Many lumbar pars fractures heal successfully with conservative treatment. Early diagnosis significantly improves recovery outcomes.
Activity Modification
Patients are advised to limit activities that place stress on the lower spine, particularly those that involve hyperextension.
Physical Therapy
A structured physical therapy program focuses on:
- Strengthening core muscles
- Improving spinal stability
- Increasing flexibility
- Correcting posture
Therapy helps reduce pressure on the lumbar vertebrae and supports healing.
Bracing
In certain cases, a back brace may be recommended to stabilize the spine and prevent excessive movement while the fracture heals.
Pain Management
Anti-inflammatory medications and guided rehabilitation may be used to manage pain and inflammation.
Many patients recover fully with conservative Lumbar spine fracture treatment in San Antonio without requiring surgery.
When Surgery May Be Necessary
Although non-surgical treatments are effective for many patients, surgery may be recommended when:
- Pain persists despite conservative treatment
- The fracture fails to heal
- Vertebral instability develops
- Nerve compression occurs
A skilled Lumbar spine specialist in San Antonio, TX, will determine whether surgery is the most appropriate option.
Surgical Treatment Options for Lumbar Pars Fractures
Advancements in spinal surgery have made procedures safer and more effective than ever before.
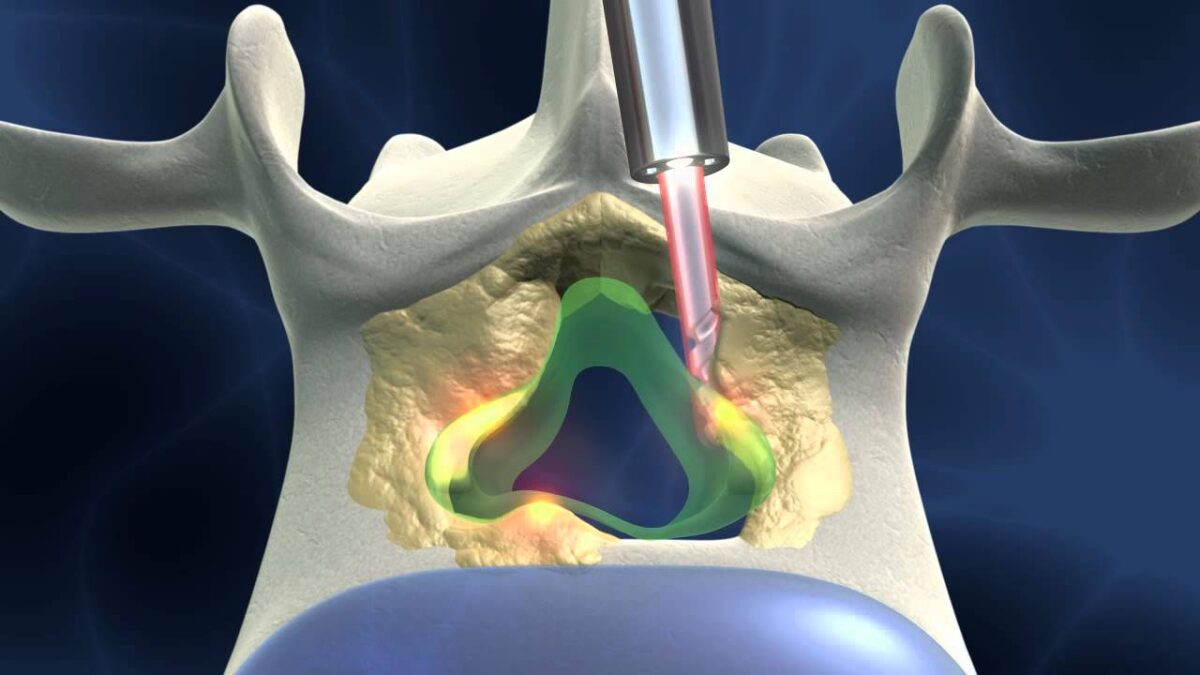
Pars Repair Surgery
When the fracture is isolated and vertebral alignment remains stable, surgeons may perform a pars repair. This procedure stabilizes the fracture while preserving normal spinal movement.
Spinal Fusion Surgery
When instability or vertebral slippage occurs, spinal fusion may be necessary. This procedure permanently joins two vertebrae together to stabilize the spine and eliminate painful motion.
Modern surgical techniques often involve minimally invasive approaches, which offer several benefits:
- Smaller incisions
- Reduced muscle damage
- Less post-operative pain
- Faster recovery times
Patients treated by experienced surgeons such as Dr. Osama Ahmed receive personalized care designed to restore spinal stability and reduce long-term pain.
Recovery After Lumbar Pars Fracture Treatment
Recovery time varies depending on the fracture’s severity and the treatment approach.
Non-Surgical Recovery
Patients undergoing conservative treatment may begin to see improvement within several weeks, although full healing can take a few months.
Post-Surgical Recovery
Patients who undergo surgery typically follow a structured rehabilitation program including:
- Gradual return to activity
- Physical therapy
- Strength and flexibility training
Following the physician’s recommendations is critical to long-term recovery.
Preventing Lumbar Pars Fractures
While not all spinal injuries can be prevented, certain habits can reduce the risk.
Maintain Strong Core Muscles
A strong core helps stabilize the spine and absorb physical stress.
Use Proper Lifting Techniques
Always bend at the knees, not at the waist, when lifting heavy objects.
Avoid Overtraining
Athletes should allow adequate recovery time between intense workouts.
Focus on Flexibility
Stretching exercises for the hamstrings and lower back can improve spinal mobility and reduce strain.
Regular check-ups with a Spine fracture specialist in San Antonio, TX, can help identify spinal issues before they become severe.
When to See a Spine Specialist
Persistent back pain should never be ignored, especially when it interferes with daily activities or physical performance.
You should consult a specialist if you experience:
- Back pain lasting more than two weeks
- Pain that worsens with activity
- Difficulty bending or twisting
- Pain radiating to the legs
- Reduced mobility
At the Brain and Spine Institute in San Antonio, Texas, patients receive comprehensive evaluation and personalized treatment plans designed to address the root cause of spinal pain.
Expert Spine Care in San Antonio
Lumbar pars fractures require accurate diagnosis and specialized care to ensure proper healing and prevent long-term complications. Early treatment can significantly improve recovery outcomes and help patients return to their normal activities.
Under the guidance of Dr. Osama Ahmed, patients receive advanced Lumbar spine fracture treatment in San Antonio tailored to their specific condition.
To schedule a consultation with a Lumbar spine specialist in San Antonio, TX, contact the clinic today.
???? Phone: (210) 625-4733
Frequently Asked Questions (FAQs)
What is a lumbar pars fracture?
A lumbar pars fracture is a stress fracture in the pars interarticularis, a small bone segment in the lower spine that helps stabilize vertebrae.
Who is most at risk for lumbar pars fractures?
Athletes, teenagers involved in sports, and individuals performing repetitive spinal movements are at higher risk of developing this condition.
Can lumbar pars fractures heal without surgery?
Yes. Many patients recover with conservative treatment such as rest, physical therapy, and bracing.
How long does recovery take?
Recovery varies depending on the severity of the fracture. Mild cases may heal within a few months, while more complex cases may require longer rehabilitation.
When should I see a spine specialist?
You should consult a Spine fracture specialist in San Antonio, TX if back pain persists, worsens with movement, or interferes with daily activities.