Chronic lower back pain can interfere with your work, sleep, and daily comfort. For many patients searching for a lumbar epidural injection specialist San Antonio, TX, understanding how this treatment works is the first step toward long-term relief. A lumbar epidural injection is a minimally invasive procedure designed to reduce inflammation and relieve nerve-related pain in the lower spine. At the Brain and Spine Institute in San Antonio, Texas, under the expert care of Dr Osama Ahmed, patients receive advanced, evidence-based treatments tailored to their condition.
This educational guide explains what lumbar epidural injections are, who may benefit from them, the procedure process, expected results, and recovery guidelines.
What Is a Lumbar Epidural Injection?
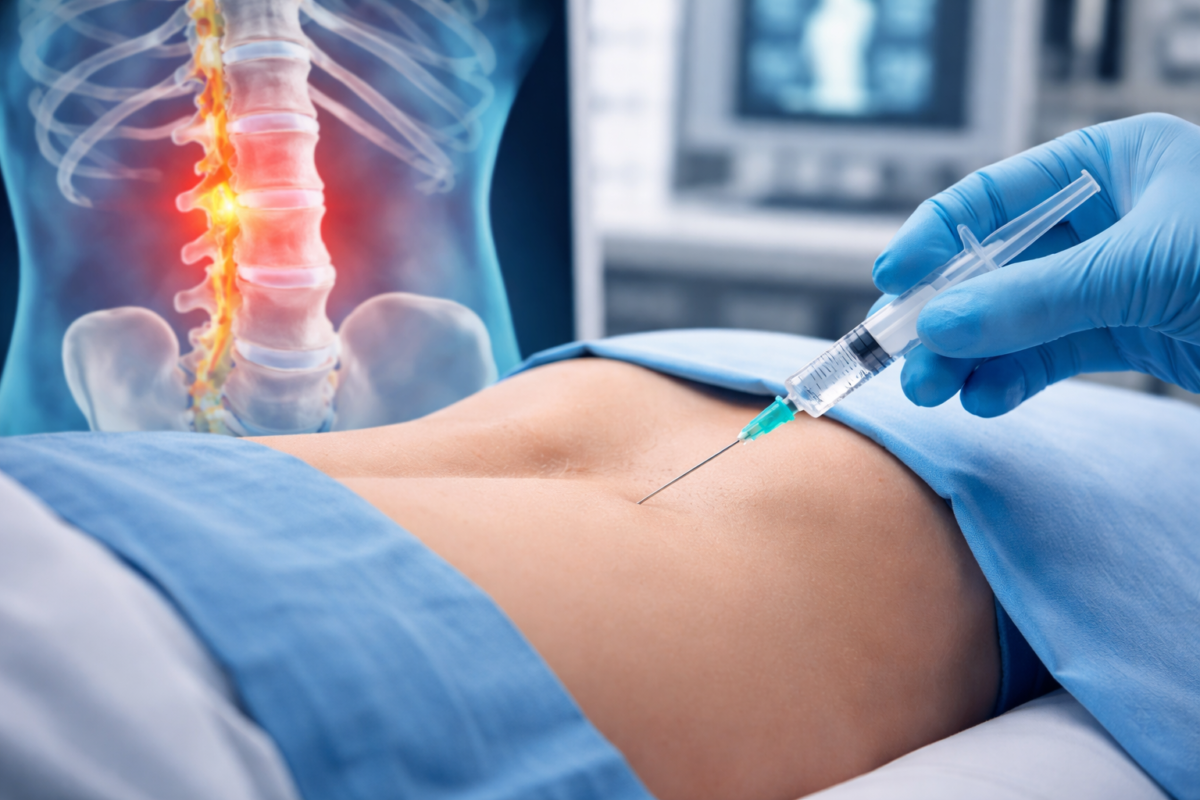
A lumbar epidural injection is a non-surgical procedure that delivers anti-inflammatory medication—typically corticosteroids—into the epidural space of the lower spine. The epidural space surrounds the spinal cord and nerve roots. When these nerves become inflamed due to injury or degenerative changes, they can cause significant pain.
The primary goal of the injection is to:
- Reduce inflammation around spinal nerves
- Relieve lower back pain
- Decrease radiating leg pain (sciatica)
- Improve mobility and daily function
This procedure is commonly recommended for patients who have not achieved sufficient relief from medications, physical therapy, or other conservative treatments.
Conditions Treated with Lumbar Epidural Injections
Epidural injections are particularly effective for nerve-related back pain. Common conditions include:
- Herniated or Bulging Discs
When a spinal disc protrudes, it can press on nearby nerves, causing sharp or radiating pain.
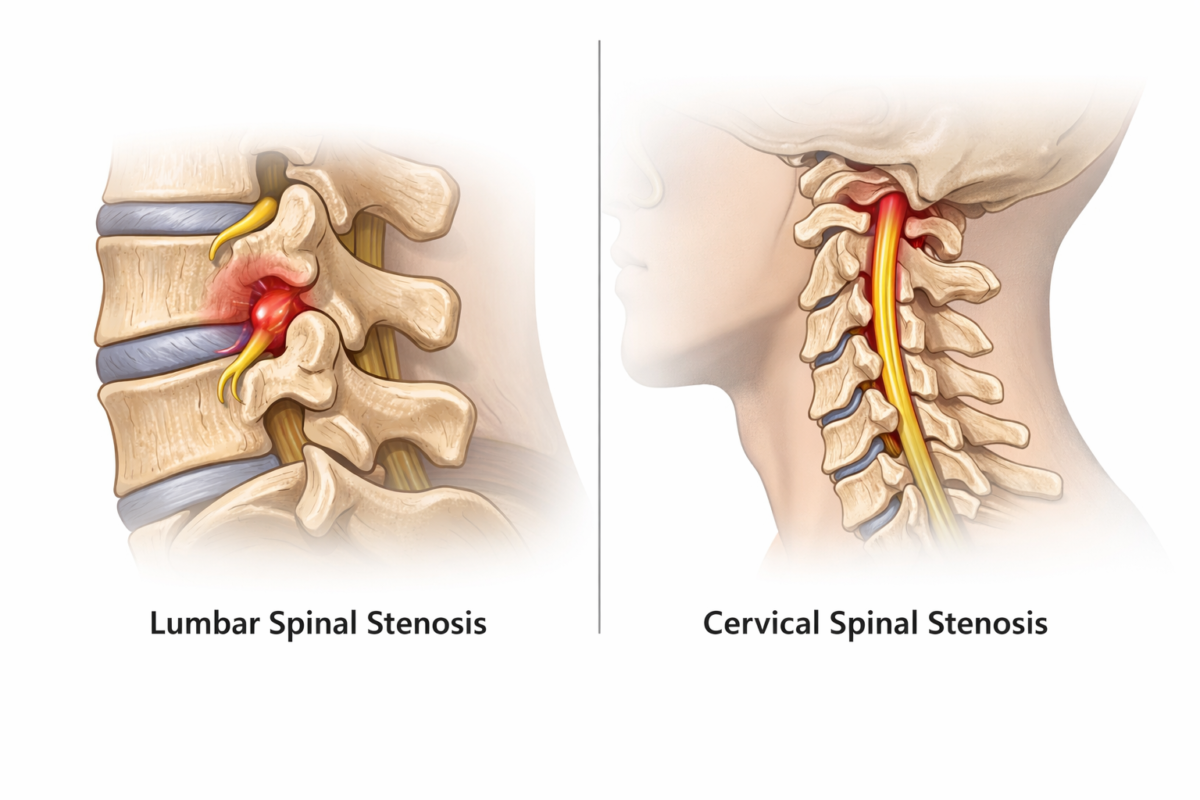
- Spinal Stenosis
Narrowing of the spinal canal may compress nerve roots, leading to lower back and leg discomfort.
- Degenerative Disc Disease
Age-related disc degeneration can result in inflammation and nerve irritation.
- Sciatica
Pain radiating down the leg due to nerve compression often responds well to epidural steroid injections for back pain in San Antonio, TX.
How Epidural Steroid Injections Work
Corticosteroids are powerful anti-inflammatory medications. When injected into the epidural space, they:
- Decrease swelling around irritated nerves
- Interrupt pain signals
- Promote healing
- Provide temporary or long-term relief
Some patients experience relief within a few days, while others may notice gradual improvement over one to two weeks.
The Procedure: What to Expect
Understanding the procedure helps reduce anxiety and ensures you are well-prepared.
Before the Procedure
- A thorough evaluation is performed.
- Imaging studies (such as MRI) may be reviewed.
- Medications and medical history are assessed.
During the Injection
- The patient lies face down or on their side.
- The area is cleaned and numbed with local anaesthetic.
- Using fluoroscopic (X-ray) guidance, the physician carefully inserts a needle into the epidural space.
- The steroid medication is injected.
The entire process typically takes 15–30 minutes.
After the Procedure
- Patients are monitored briefly.
- Mild soreness at the injection site may occur.
- Most patients go home the same day.
At the Brain and Spine Institute in San Antonio, Texas, procedures are performed with precision and safety under the supervision of Dr Osama Ahmed, ensuring optimal outcomes.
Benefits of Lumbar Epidural Injections
Many patients choose this treatment because it offers several advantages:
- Non-Surgical Approach
It provides pain relief without the need for invasive surgery.
- Targeted Treatment
Medication is delivered directly to the source of inflammation.
- Improved Mobility
Reduced pain allows patients to resume physical therapy and daily activities.
- Diagnostic Value
The injection can help confirm the source of pain.
- Potential to Delay or Avoid Surgery
For some individuals, injections significantly reduce symptoms, making surgery unnecessary.
How Long Does Pain Relief Last?
Relief duration varies depending on the individual and underlying condition:
- Some patients experience relief for weeks.
- Others benefit for several months.
- A series of injections may be recommended for sustained results.
Your response to the first injection helps guide future treatment planning.
Recovery Timeline
Recovery from a lumbar epidural injection is generally quick.
First 24 Hours
- Mild discomfort may occur.
- Rest is advised.
- Avoid strenuous activities.
2–3 Days
- Pain relief may begin.
- Light activities can usually resume.
1 Week
- Many patients notice significant improvement.
- Physical therapy may restart if recommended.
Following post-procedure instructions improves outcomes and minimises complications.
Potential Risks and Side Effects
Lumbar epidural injections are considered safe when performed by experienced specialists. However, possible side effects may include:
- Temporary increase in pain
- Headache
- Dizziness
- Infection (rare)
- Bleeding (rare)
Choosing a qualified provider, such as Dr Osama Ahmed, significantly reduces these risks.
Who Is a Good Candidate?
You may be a good candidate if:
- You have chronic lower back pain lasting several weeks.
- Pain radiates into your legs.
- Conservative treatments have failed.
- Imaging confirms nerve inflammation or compression.
Patients with uncontrolled diabetes, infections, or bleeding disorders may require additional evaluation.
Preparing for Your Appointment
To ensure the best experience:
- Bring imaging reports.
- List all medications.
- Arrange transportation home.
- Follow fasting instructions if provided.
Consulting a lumbar epidural injection specialist San Antonio, TX ensures that your condition is thoroughly assessed before treatment.
Combining Injections with Other Treatments
Lumbar epidural injections work best as part of a comprehensive care plan, which may include:
- Physical therapy
- Lifestyle modifications
- Core strengthening exercises
- Anti-inflammatory medications
- Posture correction
At the Brain and Spine Institute in San Antonio, Texas, treatment plans are customised for each patient.
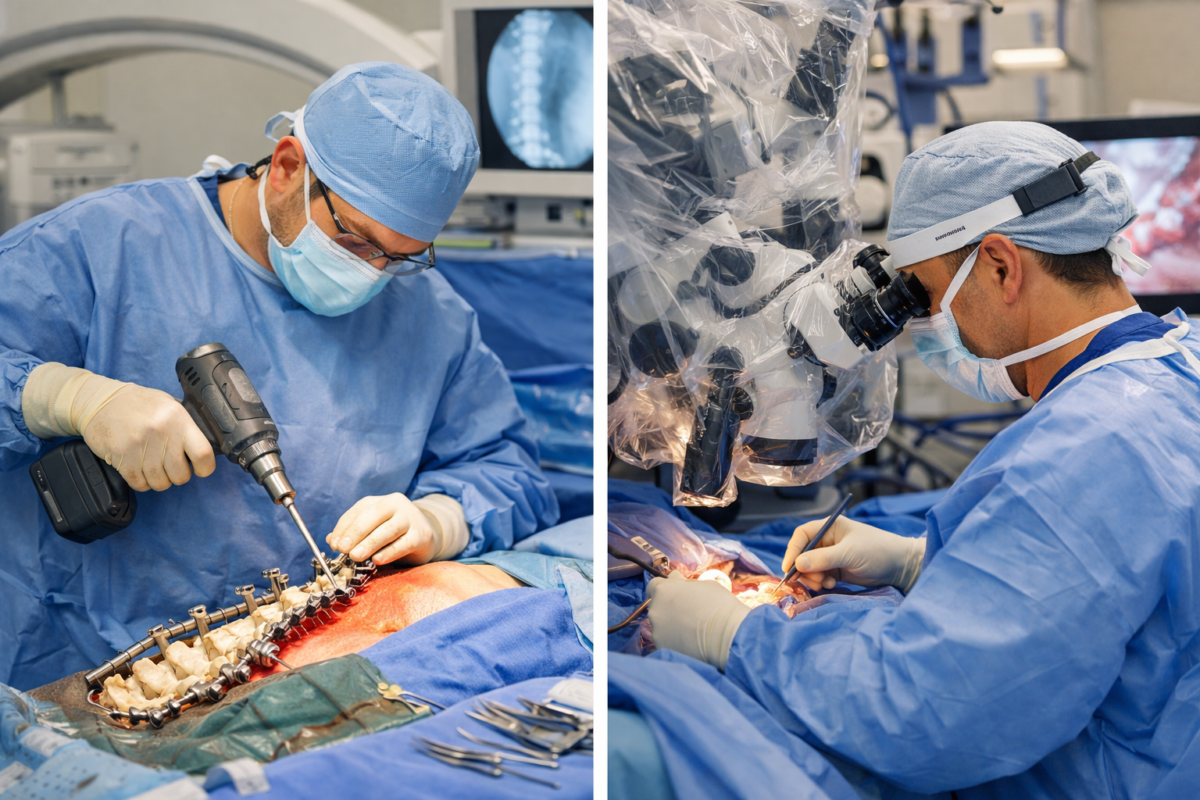
When to Consider Surgical Options
While injections are effective, surgery may be considered if:
- Pain persists despite multiple injections.
- There is significant neurological weakness.
- Structural spinal damage requires correction.
Your specialist will guide you through the safest and most appropriate options.
Why Choose Brain and Spine Institute, San Antonio, Texas?
When dealing with spinal pain, expertise matters. Under the leadership of Dr Osama Ahmed, patients receive:
- Comprehensive spinal evaluations
- Advanced diagnostic imaging review
- Precision-guided injections
- Patient-focused care
- Clear communication about recovery expectations
If you are considering epidural steroid injections for back pain in San Antonio, TX, professional evaluation is the first step.
Lower back pain can be debilitating, but modern interventional treatments offer effective relief without surgery. Lumbar epidural injections reduce inflammation, relieve nerve compression, and help patients return to an active lifestyle. If conservative treatments have not worked for you, consulting a trusted specialist can provide clarity and relief.
At Brain and Spine Institute San Antonio, Texas, Dr. Osama Ahmed is dedicated to delivering patient-centred spinal care.
Call (210) 625-4733 today to learn whether lumbar epidural injections are right for you.
Frequently Asked Questions (F&Q)
- How painful is a lumbar epidural injection?
Most patients experience minimal discomfort due to local anaesthesia. Some pressure may be felt during injection.
- How many injections will I need?
It depends on your condition. Some patients benefit from one injection, while others may require a series.
- How quickly will I feel relief?
Relief may begin within a few days, though some patients notice improvement after 1 to 2 weeks.
- Are epidural steroid injections safe?
Yes, when performed by an experienced specialist, they are considered safe with low complication rates.
- Can I return to work the next day?
Most patients can resume light work within 24 hours unless advised otherwise.
- Do epidural injections cure back pain permanently?
They reduce inflammation and relieve symptoms but do not cure structural spinal conditions.
- Is there an age limit for this treatment?
There is no strict age limit, but overall health is assessed before recommending the procedure.